The interplay of Eating Disorders and Bariatric Surgery
Bariatric surgery can be life-changing, but it can also bring emotional challenges especially if you have a history of disordered eating. The interplay between bariatric surgery and eating disorders is very significant. The prevalence of eating disorders in this population is significantly higher than in the general population. A systematic review and meta-analysis by Taba and colleagues (2021) shows that approximately 7.8% of post-op patients meet criteria for a defined eating disorder, with binge eating disorder being the most common. Loss of control eating can persist after surgery even if ‘objective’ binges decrease due to the restraints of the surgery. This looks like being unable to stop eating despite of the quantity. Grazing (repetitive/unplanned consumption of food over an extended period) ca also occur and become a problem in post-op patients
There is a strong need for psycholocial evaluation and monitoring to ensure disordered eating behaviours are identified and managed as early as possible.
Post-op eating patterns:
Eating following bariatric surgery looks like (see article by Shiri Dagan):
small portions (1 cup)
slowed pace of eating (20-30min per meal) as it allows time for the food to go through surgical changes and allow for food absorption
chewing food well: stomach can no longer break down food as it did pre surgically, so chewing becomes the first most important step
separate eating and drinking times
Medical guidelines to support safety post-op reccomend prioritizing 1)fluids and supplements, 2) protein, dairy, nuts and seeds 3)fruit & veg and healthy fats followed by grains. Added sugars, alcohol, highly processed foods or carbonated drinks should be limited because they can cause complications including dumping but also provide very little nutrition. These are general reccomendations. However, for someone with a tendency to have rigid thinking or past history of ED the issue can become that these guidelines become ridig rules driven by fear
Food Tollerance issues post-op:
Dumping syndrome happens when food moves too quickly from stomach to instestine. It can happen early (within 30min of eating) or later (1-3 hours after eating). It can cause nausea, cramping, sweating - it is more likley in gastric bypass surgery. Plugging can happen when food gets stuck.
Disordered eating post-op:
Food avoidance in bariatric surgery can be an adaptive response to avoid dumping or plugging/physiological necessity, or it can be driven by fear and eating disorder cognitions. This is where a psychological assessment/monitoring becomes very important in guiding the clinical response.
At recoverED Clinic, our eating disorder credentialed clinicians provide specialized psychological support to help you:
Psychological pre-surgical assessments
Understand and manage disordered eating patterns
Prepare mentally and emotionally for surgery
Adjust to changes in eating habits and body image afterward
Develop sustainable coping strategies for long-term well-being
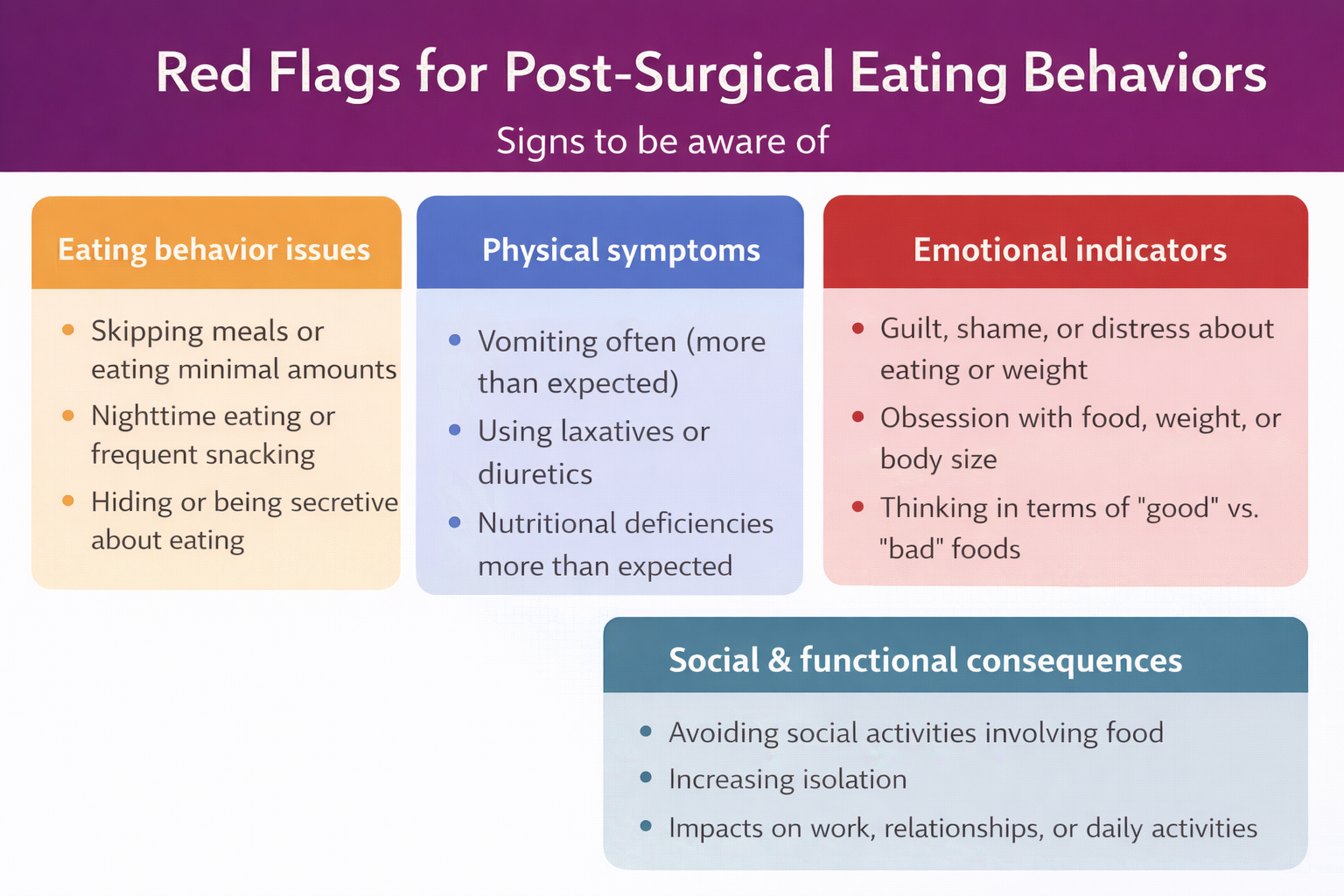
If you notice any warning signs, or would like to do some prevention work before the surgery contact us.
Note: The information provided in this blog is for educational purposes only and is NOT intended as medical /psychological advice. Please consult a healthcare professional for personalised guidance.
This blog post was created with the support of AI tools to help with clarity and structure. All content reflects the professional knowledge and clinical judgement of the authors.